WHEN Kevin Ferdinand returned from a holiday in Barcelona he did not feel well.
“On the last day I felt under the weather and when I got back to Bradford I was tired and not eating,” he says. “I have a good appetite and for me not to have that was something to worry about.”
It was December 2017, and at the time cases of Australian flu’ were on the rise, so he thought he could be suffering from that. A GP dismissed it, however, although Kevin was told that he did have a “bad case of flu’.”
“During the first few days I was not too concerned but I knew I didn’t feel right. My loss of appetite made me think it might be something more sinister,” he says. “As the days turned to weeks I became really worried.”
Previously fit and healthy, Kevin, 40, also became short of breath getting up from a chair and getting dressed. “I was even finding it difficult to brush my teeth,” he recalls.
What he did not know and what doctors initially failed to diagnose was that Kevin’s heart was failing rapidly. He was dying.
He returned a number of times to the doctors’ surgery but was repeatedly told he had flu’ symptoms. “I needed sick notes for work as well,” says the NHS data improvement officer, so I kept going back.
Then, at one appointment, a GP noticed that Kevin’s eyes were turning yellow.
“That is a sign that your kidneys are failing,” he says.
He was admitted to Bradford Royal Infirmary, where tests were carried out, with alarming results. Kevin’s heart was enlarged, or dilated, meaning that its ability to pump blood was decreased.
It was vital that Kevin be taken to a hospital that specialised in heart failure.
“They found me a bed at one in Wythenshawe, Manchester,” he says, “There they carried out more tests and realised that I had major heart failure.”
Alarmingly, just seven per cent of the organ was working. As a result, his kidneys and liver had also shut down.
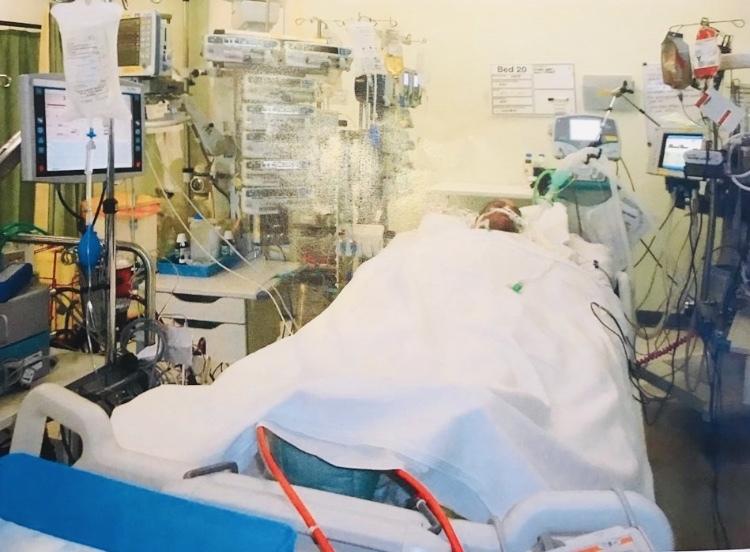
“They had all failed - I could have died at any moment,” says Kevin. “No wonder I was so exhausted. I was sent straight to intensive care where I was put on medication and drips to keep my heart stable.”
“The doctors rang my mum and stepdad in Luton who came up immediately. My dad, who lives in America, was also told. They did not tell me the full facts, so as not to alarm me, but they told my parents.”
Kevin’s heart was damaged to such an extent that the only option open to him was a transplant.
“I don’t know how long it had taken for my heart to reach that state,” he says. “The doctors could not find the cause - they did not know what type of virus I had caught.”
He was placed on life support, with a mechanical device called a BiVAD, an implantable pump connected to a machine, doing the job of his heart.
“I was not expected to live through the night, and they prepared my family for that,” he says. But live he did, remaining on the machine for six weeks.
“It was a scary time but I tried to be as positive as possible - I believe that to be very important,” he says.
He kept his spirits up by thinking of his four-year-old daughter Lacie-Rose. “I also prayed - I have a very strong faith.”
Kevin was place on waiting list for a heart, but first his lungs - one of which had collapsed - had to improve. He also had to fight off a chest infection and pneumonia.
“I had muscle wastage as well and battled my way through,” he says, praising the team caring for him.
A further setback happened when he suffered a pulmonary embolism - a blockage in one of the arteries in the lungs. “I was lucky to make it through that - they said I died about three times as they tried to save me.”
Kevin’s family visited regularly. “My dad flew over to see me which gave a lift,” he says. “I can’t imagine what it was like for them seeing me so ill.”
Not wanting her to be worried about him, he face-timed Lacie-Rose. “She would say ‘Daddy needs Calpol’,” which made me laugh.
His diet consisted mainly of soup. “I had my 38th birthday in hospital, and did manage a bit of cake then,” he laughs.
It was the beginning of April 2018 when a doctor came to tell Kevin that a suitable heart had become available.
“It was 11pm and I was just settling down for the night when the transplant coordinator came to tell me. The feeling was indescribable, but it is also a mixed feeling - you are happy for yourself, but you know that for this to happen somebody else has lost someone.”
To be compatible with a recipient a donor organ has to have the same blood type, body size and other medical factors.
The operation lasted 14 hours. “I lost 19 pints of blood during it,” says Kevin.
He woke up six days later. “When I woke up I felt as though I had been born again,” he says. “I could not wait to go out and breath the fresh air and see the sky and trees.”
He adds: “I had been in a coma for so long I had to remember how to talk and eat, and then to stand and walk.”
As he recovered Kevin felt overwhelmingly that he wanted to educate people about organ donation. “I made it my mission to pass on the message as to the importance of organ donation.”
He is now an ambassador for Yorkshire’s organ donation charity Be A Hero, speaking to others, including schoolchildren, about what organ donation means.
In August 2019 NHS Blood and Transplant recorded 493 people on the organ donor waiting list in Yorkshire.
In spring this year, a major change is taking place to the organ donation system. An ‘opt in’ scheme will operate across England, meaning that when they die, all adults will be considered a donor unless they opt out.
It is very important for families to understand each other’s wishes and feelings about organ donation and what they would
want to happen.
The charity campaigns for people to have a ‘donation conversation’ with their family, loved ones or next-of-kin, to ensure all future donations go ahead as planned.
Kevin takes great pleasure in talking to others about organ donation and what it meant for him and his family.
“Being an ambassador means such a lot to me,” he says. “I want to stress how important donation is.”
Amazingly, Kevin was back at work four months after his transplant. “I was discharged in May and had rehabilitation to get my strength back. I was back at work in August.,” he says. “I have gone from strength to strength and feel really well,” he says.
He will be on medication for the rest of his life to avoid the organ being rejected.
Recipients are not given details - other than age and sex - of the donor, but are able to send an anonymous letter to the family, which Kevin intends to do.
“I feel so much gratitude,” says Kevin. “A part of him lives on in me, and I will make sure I honour and treasure it.”
He still has to pinch himself over the fact that he is alive.
“It’s amazing that I am talking to you now. It is pretty much a miracle.”
*For more information about the Be A Hero campaign visit: leedsth.nhs.uk/a-z-of-services/organ-donation/be-a-hero/
*To find out more about the 2020 opt-out system in England visit: organdonation.nhs.uk/uk-laws/organ-donation-law-in-england/








Comments: Our rules
We want our comments to be a lively and valuable part of our community - a place where readers can debate and engage with the most important local issues. The ability to comment on our stories is a privilege, not a right, however, and that privilege may be withdrawn if it is abused or misused.
Please report any comments that break our rules.
Read the rules hereLast Updated:
Report this comment Cancel